‘He couldn’t breathe’: toddler’s ordeal shows reality of NHS waiting lists
Families who languished on NHS waiting lists for eye treatment and paediatric care for months urge ministers to move faster to clear the backlog
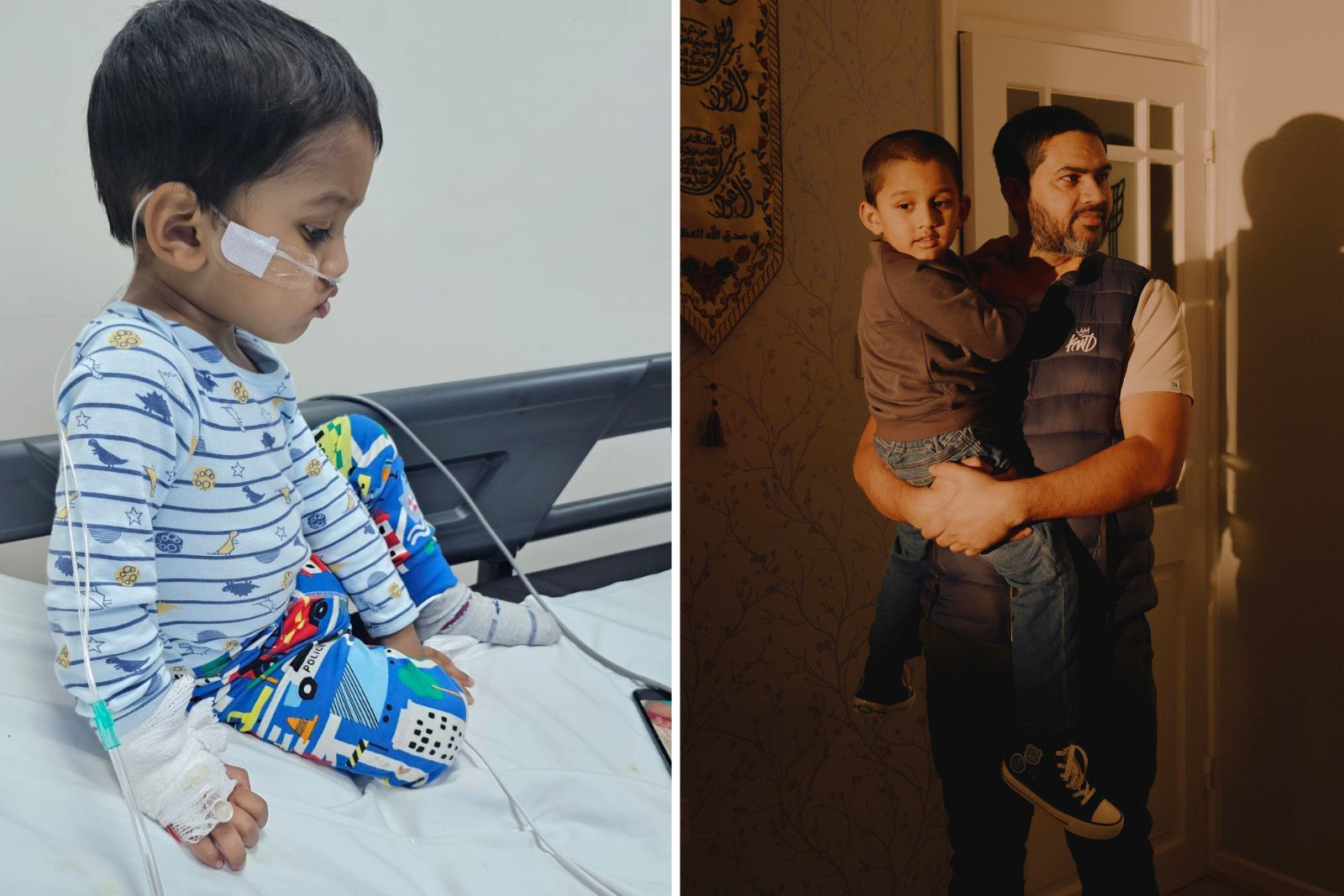
Father-of-three Junayed Malik still finds these photos of two-year-old Rayyaan — hooked up to a nasal cannula to deliver extra oxygen during an 11-night hospital stay — hard to look at.
“Every day, my son was getting worse and worse,” he said. “He couldn’t breathe properly.”
Malik had taken Rayyaan to an east London accident and emergency department in the middle of the night because he was so unwell.
Rayyaan had sleep apnoea. His tonsils obstructed his breathing and caused him to involuntarily hold his breath for short bursts of time as he slept, then wake up gasping for air.
This cycle repeated itself every minute or so throughout the night but, in the early hours of 21 October 2023, the toddler’s symptoms were even worse than usual, Malik recalled.
“He couldn’t sleep,” said the graphic designer from Ilford, east London.
“He was crying, getting crazy, banging his head to the wall. He got very angry. He was crying for a long time. I was so worried.” They dashed to Whipps Cross Hospital in nearby Leytonstone.
There, staff hooked Rayyaan up to equipment to monitor his oxygen levels as he slept — only to then have to wake him because these dropped to “dangerous” levels, his father said.
Rayyaan was at Whipps Cross for 11 nights before being transferred to Royal London Hospital in Whitechapel, also part of Barts Health NHS Trust, to finally undergo surgery.
The term “elective”, which refers to all planned, non-emergency services, does not convey the urgent reality of scenes like these, which can occur as patients wait months or even years for critically needed care. Rayyaan had been on the waiting list at a different trust — Barking, Havering and Redbridge University Hospitals NHS Trust — for planned, non-emergency tonsil surgery for seven months when these pictures were taken.
Sleep apnoea needs to be treated because it can lead to “more serious problems”, including high blood pressure, a higher chance of having a stroke, type 2 diabetes, heart disease and depression or mood changes, the NHS website states.
This family’s ordeal of waiting for planned, elective, consultant-led hospital treatment is far from unique.
Yesterday Hyphen revealed that tens of thousands of people had died after waiting longer than the recommended 18 weeks for elective procedures such as these since Labour came to power pledging to slash waiting times.

The NHS has a target — unmet since 2015 — that 92% of patients should wait no longer than 18 weeks for consultant-led elective hospital treatment. Labour’s 2024 manifesto vowed that the target would be achieved if the party won the election.
Waiting lists in England fell by more than 18,000 in December compared with those in the preceding month. But that drop — lauded by health secretary Wes Streeting as evidence that the “NHS is finally on the road to recovery” — is dwarfed by the size of the problem. Waiting lists have fallen by just 4% to 7.29 million since Labour won the July 2024 election.
Malik urged ministers to move with greater urgency to tackle the backlog.
“I don’t want any other families to get into that situation like what I suffered,” he told Hyphen.
“The government needs to move faster. These are children.”
This website reported on Monday that Asian or British Asian children were consistently more likely than those from other ethnic groups to suffer lengthy delays for elective paediatric hospital care between August 2025 and January 2026.
Our findings sparked calls from Healthwatch England, a patient safety watchdog, for NHS bosses to use demographic data on waiting lists to “drive down inequalities, including any disproportionate delays experienced by Asian children needing specialist help”. Layla Moran, who chairs the Commons’ cross-party health and social care committee, warned that many Asian Brits waiting for NHS services “suffer unacceptably inequitable outcomes”.
Lengthy delays for elective, consultant-led hospital care are also affecting adults.
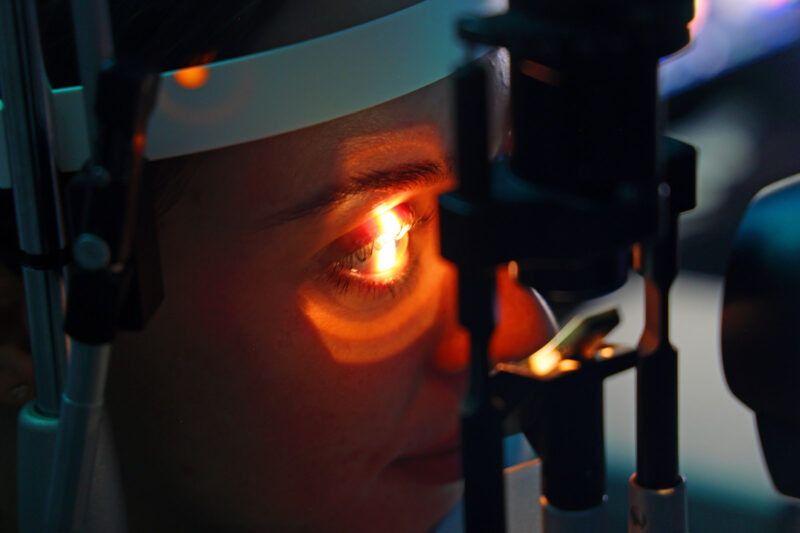
Sobrina Soloman said a year-long hold-up for cataract removal surgery left her barely able to see, as she struggled to perform daily tasks such as going to the bathroom unaided.
The mother-of-two, from Stratford, east London, had been working as a medical interpreter, often with the NHS, when she developed cataracts in both eyes in early 2021.
Her optician referred her to Moorfields Eye Hospital near central London for treatment in April 2021. A year later, she was still waiting.
“It was getting worse to the point where I couldn’t see at all,” said Solomon, 42.
“The next year, March [2022], I couldn’t see to the point people were getting me to the bathroom. I couldn’t even work. I couldn’t even look at my phone. It was that bad.”

Soloman, who has two teenage children, added: “It impacted everyone emotionally, mentally, every way. Just the other day my daughter said: ‘Do you remember you couldn’t see and we had to help you get around?’ They had to be my carers for that time.”
At its worst, she added, “if I was inside the house, I had to close the curtains because the light would affect my sight.
“My sight was like when you look through the bathroom stained glass. That’s how I saw the world.”
To regain her sight, Soloman eventually decided to pay to get the procedure done privately. This went ahead in April 2022, at a cost of about £4,000.
It took her about two and half years to pay for the surgery in instalments. According to the NHS, the procedure would usually take between 20 and 45 minutes.
“Non-urgent surgery shouldn’t be looked at as a small thing,” said Soloman.
Referring to the current backlog, she added: “It’s still happening. We don’t get the service that we deserve because NHS staff are overworked.”
Resolving the NHS elective treatment backlog has proved tricky for successive governments: the last time more patients left the waiting list than joined it was nearly six years ago, in April 2020, our analysis of the latest monthly data up to December 2025 found.
The total waiting list for elective hospital care soared during and after the pandemic, when the government paused non-urgent care to prioritise Covid-19 and emergency patients. It jumped from 3.95 million in May 2020 to a high of 7.7 million in September 2023. But demand for treatment outstripped capacity even before Covid, the British Medical Association has said.
Both the coalition and Conservative governments oversaw a period of lower real-terms growth in NHS spending compared with the Blair and Brown governments that preceded them, analysis by the King’s Fund health charity has found. A review commissioned by the current government also suggested a “desperate shortage of capital” had hindered hospitals’ productivity.
Hyphen revealed yesterday that ophthalmology — which includes treatment for conditions such as glaucoma and diabetic retinopathy, which can be more prevalent and severe among Black African, Black Caribbean and South Asian communities — was the specialism that had seen the highest number of patients die before treatment having breached the 18-week wait limit (12,403) during the three years to August 2025.
There were 592,675 patients on waiting lists for ophthalmology treatment in England as of the week ending 25 January 2026, about 60% of whom (355,280 people) were over 65.
The NHS responds
Andrew Deaner, chief medical officer at Barking, Havering and Redbridge University Hospitals NHS Trust, said of Rayyaan’s care: “We’re sorry Mr Malik and his son experienced a long wait for a tonsillectomy. There was very high demand at the time, which we’ve tackled with a targeted ‘TonKidz’ project to reduce our waiting list — treating 648 children in three months from May to August 2025.
“The wait for a tonsillectomy is now around two months.”
The Department of Health and Social Care and NHS England did not respond to multiple requests for comment.
 Newsletter
Newsletter